In mid-August, I had the opportunity to attend the 3rd annual TCOYD ONE conference – the largest conference in the world for adults with type 1 diabetes (T1D). The conference, set in the beachside paradise of San Diego’s Mission Bay, is a program of San Diego-based TCOYD.org (Taking Control of Your Diabetes). This year’s conference saw over 700 adults with type 1 from 45 states and several countries!
In short, it was amazing.
I’ve lived with T1D for almost 30 years. I first started trying to find my own kind in the wild like this about a decade ago, and it never gets old. There’s something magical about being in the physical presence of other people who live with the same chronic condition as you. The people to your right and left seem to breathe a little easier, laugh a little more freely, and move through the room a little more liberated, knowing that everyone around them inherently “gets” them. Your lunch-mates inject insulin without that subtle look-around that we do in restaurants to make sure we won’t draw too much attention to our self-care. If you run out of something, someone has a spare.
And if you find yourself with a glucose of 57 and dropping at an evening party, somebody will point out the location of the juice, casually rotate you out of view of the food spread you’d otherwise devour, and stands with you, unfazed, making conversation until you both know you’re “back.” (Completely hypothetical situation, and also, thanks, Bill.)
What else would I want to share with you? There is so much going on in diabetes research, technology, and new best practices for self-managing this condition.
In a talk by Dr. Tricia Santos, board certified endocrinologist at UCSD, we learned how to read the data coming off of our reports from continuous glucose monitoring devices like FreeStyle Libre. Which information does she recommend focusing on? She recommended looking at Time-in-Range, the percentage of time each day that your glucose falls in the range of 70-180 mg/dL. Her colleague Dr. Jeremy Pettus reminded us that every 4% is equivalent to about an hour, so more than 4% hypo means you’re spending more than an hour a day low!
Dr. Aaron Kowalski, CEO of JDRF, explained in detail the extraordinary and promising research that JDRF is funding, as well as the advocacy they continue to drive at the federal and state levels so that we can all actually ACCESS the revolutionary therapeutics and devices coming out of both academia and industry. (Disclosure: JDRF’s venture fund, called the T1D Fund, is an investor in Bigfoot Biomedical.) Kowalski described progress in Beta Cell Research — which includes Beta Cell Replacement and Beta Cell Regeneration, naming four different groups currently working on methods of encapsulation: ViaCyte, DRI Biohub, Sigilon, and Semma, describing how JDRF is leading the way in looking for new materials (metals, plastics, polymers) to continue the progress made in trying to protect transplanted insulin-producing cells from being attacked by our immune systems.
Dr. Jeremy Pettus, endocrinologist at UCSD, detailed how injectable and oral meds originally developed for people with type 2 diabetes (SLGT-2s, DPP-4s, and GLP-1s) are being explored for use (off label, and hopefully eventually approved by FDA) in people with type 1.
Pettus also delivered a moving talk on tips for living well with insulin-requiring diabetes, which included:
- Finding a great health care provider who knows what they’re doing, treats you like a person, and celebrates your successes with you.
- Gathering great tools–smart pens, insulin pumps, CGM
- Sharing and learning great new ideas with our peers from little ones like low-carb substitutions to bigger ones like “evidence-based hope”, i.e. the data shows people are living well and living longer
- Connecting with people who are rooting for you, building a community of support.
- Celebrating victories like pulling off exercise or waking up with a good number.
- Knowing when to let mistakes go, without guilt, and that it’s okay to try again tomorrow.
In breakout sessions, we learned from guest speakers like Christel Marchand Aprigliano, founder of the Diabetes Patient Advocacy Coalition, about how to work with insurance payers to advocate for your diabetes needs. She had excellent suggestions for engaging with your insurance company when you’ve had a claim denied, such as making sure you have:
- A Letter of Medical Necessity from your health care provider
- A letter from you
- Supporting chart notes and labs from your medical visits
- Peer-reviewed journal articles or clinical studies supporting use of that therapy in people like you
Some of the most interesting content of the weekend was the data presented from the T1D Exchange. Dr. Kellee Miller, PhD, author of The T1D Exchange Clinic Network and Registry: 10 Years of Enlightenment on the State of Type 1 Diabetes in the United States, presented data on just how people with T1D are doing. What are they finding? CGM makes a huge difference. Regardless of whether you use an insulin pump or multiple daily injections, people who are able to access and make use of continuous glucose monitoring, on average, have A1cs closer to the target range.
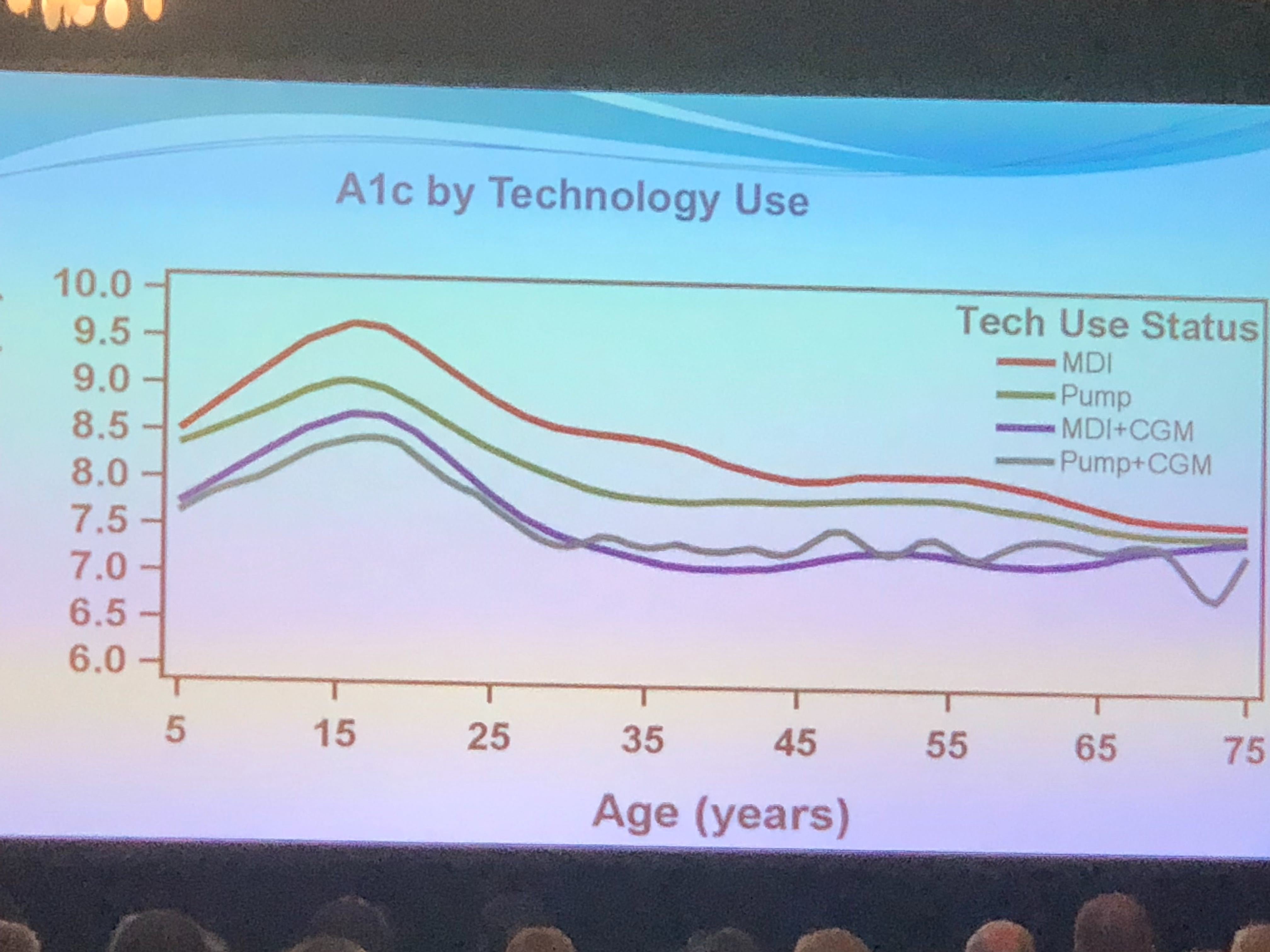
There is so much going on in T1D research and standards of care that it can certainly be hard to keep up with all of it. How do I manage to stay on top of things? I try to stay connected to organizations like TCOYD and companies like Bigfoot Biomedical–groups of people who believe that we can do better when we know better and have better tools, in the hopes we can be freer to live the lives we choose.
Have you signed up for Bigfoot's community newsletter yet? No? Sign up here!


